The Invisible Culprit: Is Histamine Intolerance Causing Your Unexplained Symptoms?
Do you suffer from a mysterious constellation of symptoms that seem totally unrelated?
Perhaps you get sudden migraines, break out in hives, struggle with bloating, or feel unexplained anxiety after eating certain healthy meals.
You might have been told it’s "just stress" or IBS, but if standard treatments aren't working, you might be dealing with a hidden culprit: Histamine Intolerance (HIT).
At our clinic, we see countless patients exhausted by this exact cycle. We understand how frustrating it is to feel betrayed by your own body—especially when you are trying to eat healthy.
Let’s explore what histamine intolerance actually is, where the excess histamine is coming from, and how naturopathic medicine can help you reclaim your health.
What is Histamine Intolerance?
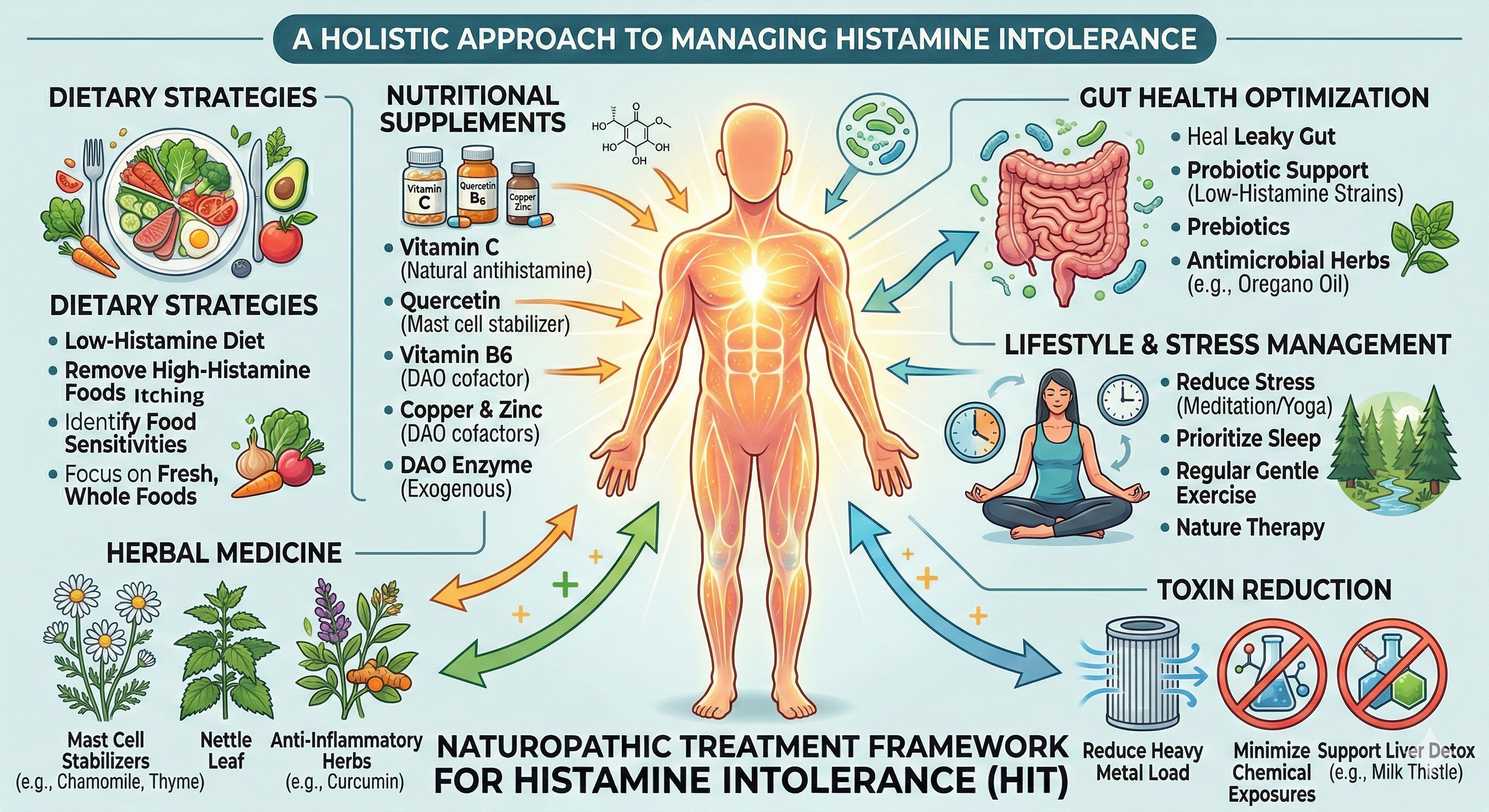
Treating histamine intolerance requires a holistic, comprehensive, and individualized plan carefully curated by your naturopathic doctor.
Histamine is not inherently bad. It is a vital chemical messenger that acts as a neurotransmitter, regulates stomach acid, and mediates immune responses. When you encounter a threat, histamine dilates blood vessels so white blood cells can quickly reach the site of infection.
The problem arises when there is a mismatch between how much histamine your body accumulates and your ability to break it down—specifically through an enzyme in your gut called Diamine Oxidase (DAO). Think of your body as a bucket. When your bucket is full, even a single drop of histamine from a piece of aged cheese can cause the bucket to overflow, resulting in a systemic inflammatory response.
So, what fills the bucket in the first place? Let’s look at the three major sources.
1. Histamine-Rich Foods (The External Inflow)
Diet is the most direct way we introduce histamine into our bodies. Histamine in food is primarily created by microbial action—meaning the older a food is, or the more it has fermented, the higher its histamine content.
Many patients are shocked to learn that their "healthy" diet is actually overflowing their histamine bucket. Major dietary sources include:
Aged and Fermented Foods: Sauerkraut, kefir, kombucha, yogurt, and aged cheeses.
Cured Meats: Bacon, salami, pepperoni, and deli meats.
Alcohol: Especially red wine and beer, which also block the DAO enzyme from working.
Certain Produce: Avocados, eggplant, spinach, and tomatoes.
Histamine Liberators: Foods that don't contain high histamine but trigger your body to release it, such as citrus fruits, strawberries, and chocolate.
(Reference: Maintz L, Novak N. Histamine and histamine intolerance. Am J Clin Nutr. 2007)
2. Gut Fermentation and SIBO (The Internal Factory)
If you have cut out histamine foods but are still experiencing symptoms, the histamine might be coming from inside the house. Your gut microbiome plays a massive role in histamine regulation.
When your digestive system is compromised by conditions like Small Intestinal Bacterial Overgrowth (SIBO) or general dysbiosis, certain strains of bacteria begin to overpopulate. Many of these bacteria (such as Klebsiella, Morganella, and certain Lactobacillus strains) naturally produce an enzyme called histidine decarboxylase. This enzyme converts the amino acid histidine from your food directly into histamine inside your digestive tract.
Essentially, if you have SIBO or dysbiosis, your gut acts as a 24/7 internal histamine factory. Furthermore, the inflammation caused by these gut infections damages the intestinal lining, directly reducing your body's ability to produce the DAO enzyme needed to clear the histamine out.
(Reference: Schink M, et al. Microbial patterns in patients with histamine intolerance. J Physiol Pharmacol. 2018)
3. Th2 Dominance (The Immune Imbalance)
Your immune system has different "gears." The Th1 pathway fights acute infections (like viruses and bacteria), while the Th2 pathway deals with parasites, toxins, and allergic responses.
In a healthy immune system, Th1 and Th2 are perfectly balanced like a seesaw. However, due to modern environmental factors, chronic stress, or chronic stealth infections, many people become "Th2 dominant."
When your immune system is stuck in Th2 overdrive, your mast cells (the immune cells that store histamine) become incredibly unstable and hyper-reactive. They begin to degranulate (burst open) and flood your system with histamine at the slightest provocation—be it pollen, a change in temperature, or emotional stress. Addressing Th2 dominance involves retraining the immune system rather than just putting a band-aid on the symptoms.
(Reference: Kidd P. Th1/Th2 balance: the hypothesis, its limitations, and implications for health and disease. Altern Med Rev. 2003)
Other Common Histamine Triggers
While food, gut health, and Th2 dominance are the big three, we also investigate several other factors that fill the histamine bucket:
Hormonal Imbalances (Estrogen Dominance): Estrogen stimulates mast cells to release histamine, and histamine stimulates the ovaries to produce more estrogen—creating a vicious cycle. This is why many women notice histamine symptoms flaring up during ovulation or right before their periods.
Genetic Mutations: Variations in the DAO or HNMT genes can genetically predispose you to slower histamine breakdown.
Chronic Stress: Cortisol depletion and elevated adrenaline directly destabilize mast cells.
Nutrient Deficiencies: Vitamins B6, C, and Copper are critical co-factors for the DAO enzyme. Without them, your body simply cannot clear histamine.
How Our Naturopathic Clinic Can Help
Histamine intolerance is complex, and standard anti-histamine pills only mask the problem by blocking histamine receptors—they don't stop the internal production or help your body clear it. At our clinic, we take a root-cause approach to empty your histamine bucket for good.
Here is how we guide our patients back to balance:
Targeted Diet Change: We don't just hand you a generic list. We help you implement a temporary, customized low-histamine diet to provide immediate symptom relief while we investigate the root cause.
Gut Rehabilitation and Supplementation: If SIBO or dysbiosis is your primary trigger, we use specific botanical anti-microbials to clear the overgrowth. We also utilize targeted supplementation, such as DAO enzymes to help digest food-derived histamine, and specific probiotic strains (like Bifidobacterium infantis) that degrade histamine rather than produce it.
Botanical and Herbal Medicines: We use potent, nature-derived mast-cell stabilizers. Herbs like stinging nettle, quercetin (found in onions and apples), and butterbur are scientifically proven to help stabilize mast cells and modulate the Th2 immune response without the drowsiness of over-the-counter medications.
Intravenous (IV) Nutrition Therapy: Because gut inflammation often blocks nutrient absorption, we offer IV nutrition therapy to bypass the digestive tract. High-dose IV Vitamin C is a powerful, natural antihistamine and mast cell stabilizer, while IV nutrient cocktails can rapidly replenish the B6 and copper needed for your body to manufacture its own DAO enzymes.
Don't Let Histamine Dictate Your Life
You don't have to live in fear of food, and you don't have to accept unexplained symptoms as your "normal." By addressing the root causes—whether it's an overactive gut microbiome, an imbalanced immune system, or a dietary overload—we can help you restore your body's natural equilibrium.
Ready to empty your histamine bucket and reclaim your vitality? Contact our clinic today to schedule a comprehensive consultation. Let's find your root cause together.
Scientific References:
Maintz, L., & Novak, N. (2007). Histamine and histamine intolerance. The American Journal of Clinical Nutrition, 85(5), 1185-1196. (Overview of DAO deficiency and dietary impacts).
Schink, M., et al. (2018). Microbial patterns in patients with histamine intolerance. Journal of Physiology and Pharmacology, 69(4). (Connecting dysbiosis and gut fermentation to histamine loads).
Kidd, P. (2003). Th1/Th2 balance: the hypothesis, its limitations, and implications for health and disease. Alternative Medicine Review, 8(3), 223-246. (Mechanism of immune imbalance and allergic propensity).
Fogel, W. A., et al. (2007). Histamine in the female reproductive system. Inflammation Research, 56(1), S45-S46. (Detailing the estrogen-histamine feedback loop).
Mlcek, J., et al. (2016). Quercetin and Its Anti-Allergic Immune Response. Molecules, 21(5), 623. (Validating botanical interventions for mast cell stabilization).
Vollbracht, C., et al. (2018). Intravenous vitamin C in the treatment of allergies: an interim subgroup analysis of a long-term observational study. Journal of International Medical Research, 46(9), 3640-3655. (Supporting IV Vitamin C as an antihistamine).